The class Arachnida comprises animal species
belonging to eleven different Orders of which only six are represented
on the Maltese Islands. Some species of the Order Acari comprising the ticks and
mites are parasitic on man and can transmit disease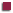 .
.
Order Scorpiones: Scorpions
 The only species of scorpion Euscorpius carpathicus found in Malta is small and has
only a mild poison which it delivers from its poison sting at the end
of its tail. The relative innocuousness of the Maltese scorpion was
remarked upon in the first published description of the Maltese Islands
Insulae Melitae by Jean Quintinus d'Autum published in 1536. Quintinus
writes that "Scorpions, fearful
animals elsewhere, are seen here innocuous in the hands of boys playing
with them; I myself saw one eating them."
The only species of scorpion Euscorpius carpathicus found in Malta is small and has
only a mild poison which it delivers from its poison sting at the end
of its tail. The relative innocuousness of the Maltese scorpion was
remarked upon in the first published description of the Maltese Islands
Insulae Melitae by Jean Quintinus d'Autum published in 1536. Quintinus
writes that "Scorpions, fearful
animals elsewhere, are seen here innocuous in the hands of boys playing
with them; I myself saw one eating them."
Order Araneae: Spiders
 With the exception of two small groups, all spiders
possess poison glands connected to their fangs. Fortunately, the fangs
of most species are too short or fragile to penetrate the skin.
Nevertheless two species of spider in Malta have been noted to be
potential problems to humans. One species - the Beady Spider Steatodo paykulliana - has been
cited as being poisonous to humans, but there have been no
cases reported of such bites occurring in the Maltese Islands.
With the exception of two small groups, all spiders
possess poison glands connected to their fangs. Fortunately, the fangs
of most species are too short or fragile to penetrate the skin.
Nevertheless two species of spider in Malta have been noted to be
potential problems to humans. One species - the Beady Spider Steatodo paykulliana - has been
cited as being poisonous to humans, but there have been no
cases reported of such bites occurring in the Maltese Islands.
 A case of a spider
bite poisoning by the Recluse Spider Loxosceles
rufescens has been reported. [Reference: D. Dandria, P. Mahoney: First record of
spider poisoning in the Maltese Islands. Central Mediterranean
Naturalist, 2002, 3(4):p.173-175: Clinical features of
locally described case: The victim initially experienced a sudden sharp
stinging pain which was followed by localized tenderness. A number of
hours later the pain increased and the bite region became indurated and
were associated with regional lymph node enlargement. This was
associated with systemic symptoms of chills, malaise, diffuse muscle
pain, low grade fever and nausea. The bite area developed a ~3 mm
haematomatous lesion surrounded
by a ~6 cm area of induration, together with inflammation of the
lymphatic vessels leading to the regional lymph nodes. In spite
of the treatment given, the local symptomatology persisted and
increased to eventually cause necrosis of the skin and subcutaneous
tissue. Clinical management: included the administration
of a systemic steroid injection together with the oral administration
of an antihistaminic and a broad-spectrum antibiotic. Surgical excision
of the devitalized tissue in the area was eventually necessary.].
A case of a spider
bite poisoning by the Recluse Spider Loxosceles
rufescens has been reported. [Reference: D. Dandria, P. Mahoney: First record of
spider poisoning in the Maltese Islands. Central Mediterranean
Naturalist, 2002, 3(4):p.173-175: Clinical features of
locally described case: The victim initially experienced a sudden sharp
stinging pain which was followed by localized tenderness. A number of
hours later the pain increased and the bite region became indurated and
were associated with regional lymph node enlargement. This was
associated with systemic symptoms of chills, malaise, diffuse muscle
pain, low grade fever and nausea. The bite area developed a ~3 mm
haematomatous lesion surrounded
by a ~6 cm area of induration, together with inflammation of the
lymphatic vessels leading to the regional lymph nodes. In spite
of the treatment given, the local symptomatology persisted and
increased to eventually cause necrosis of the skin and subcutaneous
tissue. Clinical management: included the administration
of a systemic steroid injection together with the oral administration
of an antihistaminic and a broad-spectrum antibiotic. Surgical excision
of the devitalized tissue in the area was eventually necessary.].
The
increasing interest of keeping arachnids as pets may pose some further
risk through the introduction of exotic species, e.g. Aphonopelma sp. [Tarantulas].
Tarantula venom contains a number of proteins, one of which has a
cardiovascular effect though it is highly unlikely that the bite of one
tarantula would produce a deleterious cardiac response in a human.
Clinical Features:
- SCORPION
STING: The first symptoms of a scorpion sting are that of a severe,
sharp and burning pain, similar to a bee sting. The area can become
swollen and discolored. It may form a blister. The region may
experience some paraestesia with minimal swelling, some lymphangitis
with regional lymph node swelling and an increase in skin temperature
and tenderness around the wound. The symptoms usually last for eight to
twelve hours. Scorpion toxicity is dose-related, and thus
symptomatology can be more marked in young children. A hypersensitivity
reaction is possible but unlikely.
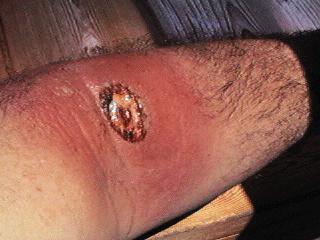 SPIDER BITE: The
bite of the Recluse Spider Loxosceles rufescens causes little pain
initially, but within two to eight hours the pain will become severe
and the area of the bite will become reddened.
The venom contains a substance that is very destructive to tissue
and causes a large spreading sore that eventually turns into a blister,
becoming dark and hard within four days. The lesion has the appearance
of a "bull's eye". Within two weeks, it forms an open ulcer that
can become secondarily infected. The bite can also cause a range
of systemic reactions including fever, chills, weakness, nausea,
vomiting, joint pains and sometimes a generalized rash or reddish
spots. Although the venom does not necessarily kill, death can occur
within the first 48 hours as a result of renal failure caused by blood
coagulation disorders leading to hemolysis and thrombocytopenia.
SPIDER BITE: The
bite of the Recluse Spider Loxosceles rufescens causes little pain
initially, but within two to eight hours the pain will become severe
and the area of the bite will become reddened.
The venom contains a substance that is very destructive to tissue
and causes a large spreading sore that eventually turns into a blister,
becoming dark and hard within four days. The lesion has the appearance
of a "bull's eye". Within two weeks, it forms an open ulcer that
can become secondarily infected. The bite can also cause a range
of systemic reactions including fever, chills, weakness, nausea,
vomiting, joint pains and sometimes a generalized rash or reddish
spots. Although the venom does not necessarily kill, death can occur
within the first 48 hours as a result of renal failure caused by blood
coagulation disorders leading to hemolysis and thrombocytopenia.
Treatment:
- The
treatment of scorpion poisoning
is largely empirical. Cool compresses should be applied to the site.
Analgesics can be given if required. Antihistaminics and
corticosteroids
are of little value.
- The
management of the Recluse Spider Loxosceles
rufescens bite poisoning should include the administration of
phentolamine to head off swelling and necrosis. Inject dexamethasone 4
mg i/m and 4 mg intradermally at the site of the bite. Repeat the local
administration after 4 hours if the area of discoloration continues to
increase in size; and repeat after 24 hours if systemic symptoms
persist. Antihistamines, and muscle relaxants may provide some relief.
Immediate excision of the bite area may be the only way to prevent
massive tissue necrosis.
- Ulcerating
lesions should be cleansed daily with peroxide; soaked in 1:20 Burow's
solution three times daily; painted three times weekly with an aqueous
triple dye mixture [1:400 gentian violet; 1:400 brilliant green; 1:1000
acriflavine].
A 5% scarlet red ointment or polymyxin-bacitracin-neomycin ointment
can be applied at bedtime. Oxygen applied several times per day to
the wound site can be of some value.
- The onset
of intravascular hemolysis can be detected early by determining
hemoglobin and hematocrit every six hours for the first 48 hours and
monitoring renal function. Any hemolytic reaction must be managed by
attempting to maintain renal function with a urine output of 200
ml/hour by giving 4-8 liters of fluid daily [orally or i/v]. Furosemide
20-80 mg orally or intravenously may be given every 4-8 hours. Urine is
kept alkaline by administering 1-2 gm of sodium bicarbonate every 4
hours. Mannitol administration may be necessary to maintain urine
output. Exchange transfusion may become necessary.




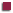


 The only species of scorpion
The only species of scorpion  With the exception of two small groups, all spiders
possess poison glands connected to their fangs. Fortunately, the fangs
of most species are too short or fragile to penetrate the skin.
Nevertheless two species of spider in Malta have been noted to be
potential problems to humans. One species - the Beady Spider
With the exception of two small groups, all spiders
possess poison glands connected to their fangs. Fortunately, the fangs
of most species are too short or fragile to penetrate the skin.
Nevertheless two species of spider in Malta have been noted to be
potential problems to humans. One species - the Beady Spider  A case of a spider
bite poisoning by the Recluse Spider
A case of a spider
bite poisoning by the Recluse Spider  SPIDER BITE: The
bite of the Recluse Spider Loxosceles rufescens causes little pain
initially, but within two to eight hours the pain will become severe
and the area of the bite will become reddened.
The venom contains a substance that is very destructive to tissue
and causes a large spreading sore that eventually turns into a blister,
becoming dark and hard within four days. The lesion has the appearance
of a "bull's eye". Within two weeks, it forms an open ulcer that
can become secondarily infected. The bite can also cause a range
of systemic reactions including fever, chills, weakness, nausea,
vomiting, joint pains and sometimes a generalized rash or reddish
spots. Although the venom does not necessarily kill, death can occur
within the first 48 hours as a result of renal failure caused by blood
coagulation disorders leading to hemolysis and thrombocytopenia.
SPIDER BITE: The
bite of the Recluse Spider Loxosceles rufescens causes little pain
initially, but within two to eight hours the pain will become severe
and the area of the bite will become reddened.
The venom contains a substance that is very destructive to tissue
and causes a large spreading sore that eventually turns into a blister,
becoming dark and hard within four days. The lesion has the appearance
of a "bull's eye". Within two weeks, it forms an open ulcer that
can become secondarily infected. The bite can also cause a range
of systemic reactions including fever, chills, weakness, nausea,
vomiting, joint pains and sometimes a generalized rash or reddish
spots. Although the venom does not necessarily kill, death can occur
within the first 48 hours as a result of renal failure caused by blood
coagulation disorders leading to hemolysis and thrombocytopenia.